Vietnam Surgical Mission Trip Report
The Vietnam experience was just incredible. I honestly think it is one of the most remarkable experiences I have ever had, and I am so appreciative that I got to go. Thank you so much again for the opportunity!
The most meaningful part was meeting the Vietnamese patients. So many of them had terrible problems — many severe neck contractures, fingers that were entirely fused to the palm, many boutonniere and swan neck deformities as well as axillary burn scar contractures. One lady’s arm was entirely fused to her body. And yet, they were some of the happiest patients I had ever met.They would literally hug me and our other team members in the mornings when we arrived; they always had big smiles on their faces and were laughing. One of the first patients we did was a lady with popliteal fossa burn scar contractures that were so bad she couldn’t walk, so one of her family members literally carried her everywhere. She started crying when she woke up from surgery because she was so overwhelmed that her legs were finally straight after all these years. It was incredibly heart-warming to be a part of this! I was sad to leave at the end of the week.
Beyond that, from an educational perspective, I had a wonderful experience. I worked with Dr.Robert Bibi from New York and Dr. Kim Bjorklund, a hand surgeon who will be working atUniversity of Indiana next year. They were both very intent on teaching, and they were essentially walking me through almost all of the cases. I really enjoyed the boutonniere corrections and rebalancing the biomechanics of the fingers. All in all, our team operated on 35 patients, 20 of which I was able to help myself.
Finally, I really enjoy experiencing new cultures, and Vietnam was a world away from any place I had been before. The people were incredibly friendly. We worked in conjunction with the Cho Ray Hospital staff and surgeons, and the American and Vietnamese teams were teaching each other the opposite language. By the end of the trip, I think I had learned all of the common names of surgical instruments in Vietnamese. It was a collaborative environment, and we were able to benefit from learning from each other while providing high quality patient care.
Thank you so very much for the wonderful opportunity – really, I believe it was one of the most meaningful experiences I have ever had, and I am truly grateful for it. I hope to be able to go back one day.
Trip Report | Ho Chi Minh City, Viet Nam, April 5 -12, 2014
Surgical Volunteers International (SVI) in partnership with Wonder Works, Americares and Map International has just returned from a week-long mission trip to Ho Chi Minh City, Viet Nam, April 5 -12, 2014. There we worked in Cho Ray Hospital, a large government hospital with an estimated 2800 beds, providing general medical and surgical care with all the usual specialties and sub-specialties. HCM City/Saigon is the largest city in Viet Nam, and the Burn Unit at Cho Ray is the largest and busiest in the country.
We worked in the Department of Burns and Plastic and Reconstructive Surgery. This department is headed by Dr. Doan Dao and has both full-time and volunteer surgeons on the staff. This trip marked the fifth time SVI has been a guest of this department and carried out surgery for the correction of burn scar deformities under the auspices of, and with the assistance of, Dr Dao and his staff.
The SVI team on this mission consisted of 10 people, with the following distribution of labor: anesthesia (2), plastic surgeons (2), operating room/surgical assistant nurses (2), recovery nurse (1), floor nurse/patient coordinator (1) and team director/RN (1). A young surgeon from Cairo, Egypt, in his final phases of plastic surgery training, completed the team and functioned as surgical assistant.
The work began with a screening clinic on Saturday April 5, at which time approximately 55 patients were examined and evaluated for possible surgery. Of those seen, 36 were selected and worked into the operating schedule for the following week.
Burns are literally the scourge of the developing world. They are endemic in many countries visited by teams like ours. Statistics are hard to come by, but anecdotally the incidence is high and the devastation to life and limb tragic. The damage done to the patient, family and community is incalculably overwhelming.
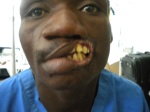
Sources of the burn injuries we encountered included house fires, cooking fires, gasoline fires (accidental), hot water, electrical burns, and perhaps saddest of all, chemical burns by the intentional throwing of acid onto a person’s face and chest. One patient seen in our clinic had intentionally doused himself with gasoline and lighted himself afire. He had nearly total-body burns and yet had survived.
The types of deformities we saw and subsequently operated on included contractures of nearly all joints and movable body parts. One of the most common was the contracture of the chin and neck down onto the upper chest, often with dystopia (pulling downward) of the lower lip and mouth. This often was in the form of a thick collar that prevented almost any kind of movement or lifting of the head. As one might imagine, eating and drinking and control of one’s own saliva were an issue for these patients.
Other problems included deformities of the hands and fingers, in some instances so severe that the fingers were drawn backward onto the dorsum or back of the hand. Often digits were missing or only present as stumps. Similar deformities were found in the feet. Several patients had suffered amputations the hands, arms, feet and legs, either by the mechanics of the fire or burn itself, or by necessary surgical intervention as part of their primary care.
Other problems included absent or deficient eyelids with an eye at risk, microstomia or smallness of the mouth such that one could hardly eat, absent ears and noses, and finally painful scars and open sores from the fragile tissue of the healed burn scar.
In total 36 patients were operated on, some with more than one surgical procedure carried out. Most of the procedures were some type of scar excision and release, and most required skin grafting for coverage. Z-plasties were incorporated into several of the closures. Eyelids were reconstructed and grafted, but on this trip no attempt was made to reconstruct ears or noses, complicated procedures requiring long-term planning and repeat procedures. Also most of the complex hand problems were deferred to a visit some months hence by a team from elsewhere coming to do specifically hand surgery.
We worked closely with the local team, including surgeons, nurses, and anesthesia. They are all excellent in their respective areas of care and expertise. They are just nearly overwhelmed by the sheer numbers of patients and the magnitude of the injuries brought to their front doorstep.
Three additional cases were performed by a talented and clever surgeon who has developed a neat little regional arterialized flap for correcting axillary (armpit) contractures. On another couple of cases, the finesse of the local surgeons with the Humby knife for freelance skin-grafting was ably demonstrated.
This team of SVI volunteers worked competently and compassionately, tirelessly and professionally, laced with good humor and laughter, to carry out the demands of this week. The local team of doctors and nurses gave freely of their time and talents and never once complained about the extra burden of work we brought to them.
The finale of the week was a farewell dinner held at a down-home but elegant small restaurant, where our team was hosted by Dr Dau and his staff of doctors and nurses, and we were given nice memorial gifts as tokens of their thanks for a hard job well done.
The team then bid each other farewell and departed for their various routes to return home and their various daily lives…all touched by the experience of the past week and in particular by the courage and gratitude of the patients for whom we had worked.
mes 13 Apr 2014
VN Trip Report- Cho Ray Hospital, Ho Chi Minh City, Vietnam
Surgical Volunteers International has completed their fourth surgical mission to Cho Ray Hospital in Ho Chi Minh City, Vietnam. We were invited to the hospital by DR Doan Dao the director of the hospital burn unit and Dr Nguyen Son the hospital director. The volunteers came from all over the US but we also had two from India.
CRH is a 2,800-bed referral hospital and serves patients from all the provinceŐs in South Vietnam and also receives some patients from Cambodia as well. The burn center is the only unit in the South of Vietnam and is extremely busy. They always have a full unit with upwards of 70 burn patients.
We arrived at the on Saturday June 22, 2013. 80 patients waiting to be screened for surgery greeted us. All the patients were past patients at the center and had debilitating contractures. After all the patients were screened we identified 33 of the patients that we felt could most benefit for a surgical procedure. I have a list of about 20 patients that we would like to do on our next trip.
On Sunday most of the team went on a tour of the Mekong Delta region. They departed at 8 AM and returned at 5 PM. The trip not only provided a tour of the countryside it allows the volunteers to get out of the hustle and bustle of HCM.
Surgery began early on Monday morning and proceeded until early Friday afternoon. We were able to provide surgical treatment to 33 patients. Lots of Full thickness skin grafts. All the patients did well.
During the week I was invited to visit a hospital in Bien Hoa Province. They are going to open a burn center there and will be sending nurses and doctors to Cho Ray Hospital for training. They have requested that SVI brings a team there next year.
At the end of the mission I took a bus to Phnom Penh, Cambodia. I was met by DR Sin Moth the Deputy Director of Cho Ray Phnom Penh Hospital. The hospital is a joint project between the Cambodian and Vietnamese government. It is scheduled to open in September 2013. SVI is exploring how we would best be able to assist them once they are open.
For the remainder of this year we have a Health Fair clinic scheduled in St Vincents, and clefts missions to Haiti and Brazil. I will be adding missions for 2014 as soon as dates and locations are set.
Cho Ray Hospital, Burn Unit 2012
Surgical Volunteers International has completed its third trip to the Burn Center in Cho Ray Hospital. The team arrived in Ho Chi Minh City for patient screening on March 31st. As always we stayed at the Bat Dat Hotel which is about 15
minutes walk from the hospital.
The team consisted of 12 volunteers with 2 surgeons, 2 anesthiologists, 1 CRNA, 1 medical student, and 6 registered nurses. Everyone was from the US except for one surgeon who joined us from Egypt.
Cho Ray Hospital is the largest hospital in the South of Vietnam. It has 1700 beds and 2800 patients. The burn center had 112 patients the week were there. Some rooms had up to 10 patients with stretchers parked right next to each other.
Thirty-nine of the patients had been admitted for surgery by the SVI team and the rest were recovering from recent burns. In spite of the crowded conditions the patients all were receiving excellent care from the Vietnamesestaff. Daily baths and dressing changes were the norm. The unit is clean and tidy.
Due to a Vietnamese National holiday on Monday we did not begin operating until Tuesday. Even with the shortened week we were able to provide surgery for every candidate we screened on Saturday.
A total of 39 received life changing surgery during the week. Many patients had severe burn scar contractures of the hand that made it impossible to perform even the simplest of tasks. We also did several neck and axillary contractures.
One patient had burn scars that had left his legs in a sitting position. Hopefully he will now be able to walk.
I would like to once again thank our hosts and the Volunteers. The week was one of hard work,excellent care and compassion for those suffering from debilitating contractures.
Egypt 2011 Mission Report
On September, 30th 2011, Ain Shams University Hospitals in Cairo, Egypt received the well-trained and enthusiastic Surgical Volunteers International team, the team consisting of dedicated 13 advance medical stuff arrived at Ain Shams University Guest House early Friday morning following their mission to Mansura Pediatric hospital, A detailed discussion of the week’s agenda was held with an agreed upon 7:30 AM daily start time throughout their mission trip, and the anesthesiology team members went to the operative theater to set up the operating rooms for the quick start the next day, On October 1st ,2011, we held a joint clinic where we screened over than 100 cases of 1ry and 2ry cleft lip and palate cases, the clinic was composed of 3 stations one for surgeons, the two others for pediatrician and anesthetists, the clinic went really well and 70 cases were scheduled for surgery for the rest of the week, we started our operative day one on October 2nd, at 7:30 AM, we operated on 18 cases and we finished at 6:30 PM, the workload was pretty the same the next days, by October 5th the total no. of surgeries performed extended to 58, surgical volunteers performed most of the surgical procedures and assisted local doctors in many others, nearly all the medical supplies were provided from the SVI, as well as postoperative medications, we thank all the team members for providing us with the opportunity to work collaboratively with them on this medical mission, and for their extraordinary personal sacrifice of time, effort and money .
Presurgical orthopedics in cleft/craniofacial care
The current state of the art in treatment of cleft lip/palate is using presurgical techniques, in order to allow for a more conservative surgery and better clinical outcomes. However there are currently no groups that provide this in the countries we visit, mostly due to financial, logistic and training limitations. Therefore, at SVI we have decided to make an effort to provide these services in order to increase the quality of care to our patients.
The first part of the protocol will be implemented in Cairo this year
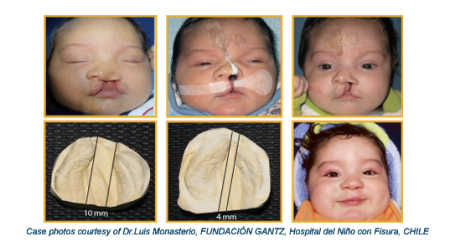
We believe that as a result of providing presurgical orthopedics, we will have:
1. Less invasive surgeries
2. Better healing time
3. Decreased amount of revisions required
4. Decreased amount of complications
Additionally, we are making an effort to improve our patient tracking system. Part of this tracking system will include systematic record taking, which will allow us to conduct outcomes assessments on how we can best serve the local population.
Another area of need is teaching the local health care practitioners the newer techniques in cleft care. We are increasing our emphasis on teaching, and hoping to provide visiting scholarships for local doctors to visit some leading Centers in the U.S.
What exactly is presurgical orthopedics?
There are 3 components of presurgical orthopedics, and depending on the severity of the case, each component may or may not be employed
1. Extra-oral taping. This is done for the cleft lip, and:
Gently guides soft tissues and bone into a better position for a cleft
lip repair under less tension.
Allows one to approximate the soft tissues of a cleft lip
Allows for a controlled force to re-position the prolabium and premaxilla to allow for a less invasive surgery
May eliminate need for early lip adhesion surgery.
Relieves tension on sutures when used post-operatively.
2. Alveolar molding. This is done for the cleft palate, and:
Decreases width of palatal cleft
Decreases amount of scar tissue
Decreases likelihood of oro-nasal fistula
May help in feeding by acting as an obturator
3. Nasal stent. This is done for the nose/columnella, and:
Improves nasal tip, nasal symmetry, and columnella length
Decreases deformity of the nasal cartilage
This information was partially taken from the following website, which also has before and after pictures:
http://www.canica.com/dynacleft.asp
You can also become a sponsor
$40 provides extraoral taping and nasal stent for a patient
$30 provides nasoalveolar molding for a patient
If you would like to help in this effort, or if you have any questions or comments you are welcome to contact:
Mairaj Ahmed, DDS MS
Assistant Professor, Mount Sinai School of Medicine
Section Chief, Orthodontics & Dentofacial Orthopedics
Cleft/Craniofacial Team Orthodontist
Mount Sinai Hospital
One Gustave L. Levy Place, Box 1187
New York, NY 10029-6574
Tel: 212-241-0300
Fax: 212-996-9793
mairaj.ahmed@mountsinai.org
Haiti Days 5 & 6
We have finished most of the palates, as it is better to do these earlier in the week incase they have any postoperative problems with airways.
The haitian nurses, who have been our scrub nurses on this trip, are doing very well and are improving daily.
Haiti Days 3 & 4
Today we completed our second day of operating. On day one, we did 6 lips. Today we did 3 lips and 3 palates. Everything went well. It’s very hot in the ORs, but sometimes we find pockets of air conditioning that feel just fantastic.
The TCH pediatrician who is also here with us, Elizabeth Montgomery, has been spending the days at the “Sean Penn” camp, in their pediatric clinic/hospital and happened to deliver a baby girl today! She is seeing a lot of the illnesses here that we learn about but never really see in the states, like rickets, and also a lot of GI illnesses and scabies.
Out host, Lance, returned home today. He is an American businessman who employs 500 haitians in his factory that makes small electronics. When the earthquake happened, to help these people keep their jobs, he provided full meals for his employees when at work, including one to take home for their families.
Haiti: Days 1 and 2
We arrived in PAP on Saturday afternoon. After gathering all of our supplies, we piled into our van and headed to the hospital. Upon arrival, there were already 4 or 5 ladies with newborn babies with clefts waiting for us. We unpacked the supplies and headed up the mountain to the home we are staying at. Passing through the main area of PAP was as expected… Tons of tents, rubble in street, and just so many people. Next we passed through petionville, and finally up the mountain to Fermathe. We are staying at the home of a Haitian couple, Nadia and Lance Durban. We had a very homemade dinner.
Today we woke up and realized the beauty of where we are staying. The view is gorgeous and there are avocado trees and wild orchids growing off trees. Very peaceful and quiet.
At 8 am we went down to the hospital for patient screening and prepping the ORs. There are also two inpatient areas, in addition to the ORs and recoveery rooms. About 50 patients were waiting… Mostly with cleft lips. The screening took the entire morning. Patients had traveled from over 5 hours away. One little girl had on a white party dress with white eyelet socks and dress shoes. Adorable. We had to say no to a few patients, mostly patients with vascular malformations, for which we did not have the right treatments. We will definitely bring some sclerosing agents on the next trip. The other patients that we couldn’t offer treatment for were those that were too small- younger than 9 mo or 20 lbs.
Things began to wind down and we were gathering our belongings, when we noticed that a bench we had been sitting on 10 minutes earlier was now occupied by a small body covered in white sheet. It’s one thing to see a picture of it and it’s a completely different thing to see it.
We have 36 on the schedule for this week and will start operating tomorrow AM.